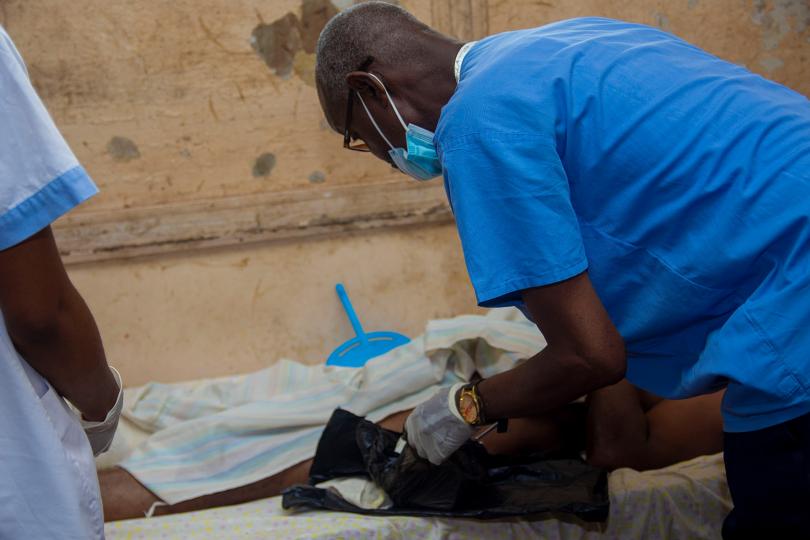
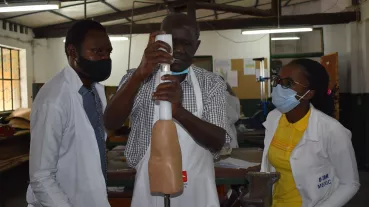
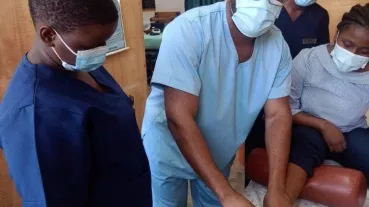
Developing Safe Surgery Practice in Kongo Central Province, Democratic Republic of Congo

Situation:
Compared to the conflict-affected East of the country, the South West has received little attention from the international community, and yet the health needs of the population are great. International assistance is largely focused on the prevention and management of infectious diseases, however, the burden of disease requiring surgical intervention-such as trauma, cancer, infection,and complications from childbirth-is substantial and growing. Surgery is an integral component of any properly functioning healthcare system. In Kongo Central province, most of the population of 6 million people lack access to safe, timely and affordable surgery. For patients who are able to access surgical care, peri-operative mortality and complications are high and outcomes are poor. The barriers to accessing safe surgery in Kongo Central include: the risk of financial hardship for patients, the lack of a trained healthcare workforce, poor infrastructure and equipment, and weak strategic leadership. The four main tertiary hospitals in the province employ experienced surgical staff, but there is only one full time post-graduate trained surgeon for the province. These hospitals rely heavily on medical officers without postgraduate surgical training for the delivery of emergency surgical care. With limited specialist expertise concentrated in large urban centres, safe surgical care is out of reach for the rural population, who are often the poorest in society. In the district health centres, non-specialist staff,such as recently qualified doctors,nurses and midwives,routinely conduct procedures like C-sections, laparotomies, wound closures, and management of open fractures with little or no supervision. The current lack of capacity at district health centreshas a negative impact on the effectiveness of the health system. If tertiary hospitals are overcrowded and burdened with acute surgical volume from the district level, they lose the ability to offer more complex surgery and, elective surgery. Communication between district health centres and the tertiary level is poor, resulting in inappropriate referrals and unsafe handover of patients.
Objectives:
The objective of this project is to improve surgical outcomes for rural and urban communities in Kongo Central Province of DRCongo. In partnership with the Provincial Ministry of Health, and through training delivered by teams from tertiary hospitals, we will increase the skills, confidence and working environment of health workers in the practice of safe surgery. A complementary mentorship programme will foster stronger communication between the tertiary, district, and provincial levels of the health system.
• Number of operations per month using the WHO checklist
• Percentage of trained health workers with improved skills and knowledge of safe surgical practices at 8 target health facilities
• Number of health workers from tertiary facilities attending Training of Trainers (ToT) on safe surgical practices
- We will provide training and support for the largely non-specialist workforce at district level and will refresh the skills of health workersat the tertiary level
- We will support the establishment of a mentorship programme, which twins health workers from tertiary hospitals and district health centres. These interprofessional relationships will increase the confidence, knowledge, and skills of non-specialists at district level, enabling them to assess patient risk and make safer, more informed decisions in relation to stabilisation and transfer of the patient.
- We will increase capacity for leadership, evidence-based decision making, and strategic planning at the provincial level by working with health facilities to collect and report on a minimum set of surgical related data. At the provincial level we will support leadership to understand and use the new data in workforce and resource planning.
- Lastly, we will produce collaborative research on surgical capacity and caseload across the facilities that will enable us to demonstrate impact.
Since the inception of our DRC partnership in 2013, our goal has been to work in genuine partnership with Congolese healthcare facilities, provincial government and medical schools to develop sustainable approaches to emergency and essential surgical care. We have designed the project in close collaboration with colleagues in the Provincial Ministry of Health, to ensure its appropriate and addresses the needs on the ground. This is important for buy-in and fostering ownership of project activities for key stakeholders in the health system. In particular, this project will support the increase in capacity of the Provincial Health Division as well as improving collaboration and communication between District and Tertiary health departments by establishing a programme of coaching and mentorship between them. The project will also improve health workers skills in surgical data collection and will increase the capacity of the Provincial Health Division to understand and use the new data for evidence-based decision making in workforce and resource planning, improving quality and efficiency at the Provincial level. The long-term partnership between KGHP and Kongo Central partners ensures strong Congolese ownership, which is key to sustainable change.
- This project is building on a long-term partnership and existing work, furthering the capacity of individuals we have previously trained, supporting them with knowledge and skills on how to train others, as well as create mentorship relationships that will enhance cooperation between different levels of the health system in the province. In addition to the collaborative research activities on surgical capacity, peer-to-peer learning is built in the design and fostered throughout the project.
- We know that safety in surgery needs the reliable execution of multiple necessary steps in care, not just by the surgeon but by a team of healthcare professionals working together for the benefit of the patient. This is why we will include all members of the multidisciplinary team (surgical, anaesthetic, nursing, allied health professionals) in our training and maintain a particular focus on gender parity in our activities.
- The last innovative element of our project is incorporation of environmental sustainability in our equipment purchases, with the aim of reducing environmental impact of surgery; by using ecoclaves and equipping operating theatres with solar lights.
Here you can find further information.