
Bad Homburg v.d. Höhe, January 31, 2024 – For physicians who take a longer time-out for family- or care-related commitments, the decision in favor of parental leave, child care or caring for relatives poses an obstacle to further advancement of their academic careers. Commitments like these are viewed as one of the reasons why, on average, women in Germany reach top academic positions less often. In light of this situation, in 2023 the foundation Else Kröner-Fresenius-Stiftung (EKFS) announced a call for applications for the first time to apply for a flexibly designable reentry program in the field of medicine. The individually deployable funding resources amount to 400,000 euros in each case. Out of a total of 64 applications submitted, three physicians were chosen to receive funding.
The aim of the call for applications is to enable an effective reentry and the continuation of a promising career for physicians who are particularly successful in the clinical and research sectors, both women and men, subsequent to a longer family- or supervisory care-related phase by utilizing flexible and individually deployable funding. “By doing so we not only want to help a group of disadvantaged individuals, but also alleviate a deficit of excellently trained and outstanding scientists that is disastrous for the German research and science system,” explains Prof. Dr. Michael Madeja, Chairman of the Management Board at EKFS.
The call for applications addresses physicians at university hospitals in Germany who have attained their doctorates or postdoctoral teaching credentials, and who had completely interrupted or significantly reduced their clinical and research activity to the detriment of their research in favor of a family phase lasting at least one year and involved a maximum of three years. The return to the clinical and research sectors accompanied by employment in an at least 80% FTE position must take place by April 30, 2024 at the latest. Within the scope of this funding, at least 50% of the work hours ought to be made available for research.
The following research projects are intended to be realized using the funding awarded:

Ovarian reserve disorders – Analysis of genetic determinants: PD Dr. Julia Rehnitz, Heidelberg University Hospital, Pregnancy & Gynecology Unit, Dept. of Gynecological Endocrinology and Fertility Disorders
For female fertility, the ovarian reserve and the maturation of oocytes (egg cells) in their follicles (oocyte and surrounding somatic cells) in the ovary is a decisive factor. Disorders within this process (oocyte maturation and folliculogenesis disorders) can express themselves as premature ovarian insufficiency or in the form of a poor response to a hormonal treatment for infertility. The goal of this project is to identify molecular genetic correlations and detect potential genetic causes and determinants in terms of folliculogenesis disorders and ovarian reserve disorders in order to be better able to adapt and improve the prognosis and therapeutic options in the future for women who wish to have children.
PD Dr. Rehnitz works in a capacity as senior physician in the Department of Gynecological Endocrinology and Reproductive Medicine, Pregnancy & Gynecology Unit at Heidelberg University Hospital. She heads the work group Germ Cell Research on Folliculogenesis and Disorders Thereof. She has three children of her own and returned to her department upon conclusion of her last parental leave at the end of October 2023. “After returning from my parental leave, the funding from EKFS allows me to carry on my years of painstakingly built-up research in my work group with the personnel strength, time and financial security needed to achieve this,” reports PD Dr. Rehnitz.
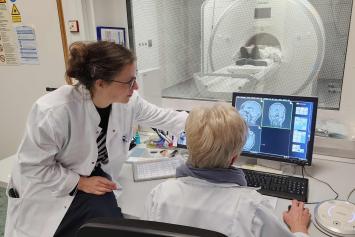
New classification systems and biomarkers for cerebral small vessel diseases:
Prof. Dr. Stefanie Schreiber, Dept. of Neurology, Düsseldorf University Hospital and Heinrich Heine University Düsseldorf
Cerebral small vessel diseases (CSVD) are among the most significant causes for strokes and forms of dementia. For the hypertensive or amyloidogenic variant, i.e. based on high blood pressure or pathogenic protein deposits (plaques), the risk, progression, prevention and therapy vary. Within this project a precise classification of these variants that has not been available until now is supposed to be established for clinical practice by means of new imaging markers, e.g. regarding vascular wall integrity, inflammation and neural networks. In a corresponding mouse model the project group around Prof. Dr. Schreiber is going to study new blood biomarkers for cerebral small vessel diseases on a parallel basis, integrate them into the classification scheme and bring them into application on patients.
After studying medicine in Magdeburg, Germany, Prof. Dr. Schreiber completed her clinical and scientific training as neurologist and neuroscientist in Hanover (Germany), Southampton (UK) and Berkeley (USA). She is currently senior physician in the Departments of Neurology at university hospitals in Düsseldorf and Magdeburg, as well as head of a work group at DZNE, the German Center for Neurodegenerative Diseases. “As a mother of five children, this special funding makes it possible for me to continue to forge ahead with my research on cerebral small vessel diseases with the aim of developing new possibilities for prevention and therapy,” Prof. Dr. Schreiber points out.

Development and evaluation of new pathophysiologically relevant scores for predicting acute graft-versus-host disease and survival following allogeneic stem cell transplantation: Prof. Dr. Daniela Weber, Dept. for Internal Medicine III, University Hospital Regensburg
Acute graft-versus-host disease (aGvHD) of the intestinal tract represents a serious and sometimes life-threatening complication of allo-SCT. A loss of bacterial diversity in the intestinal tract plays a key role in the way aGvHD manifests itself and influences survival following allo-SCT. It is therefore of central significance to recognize changes in bacterial composition at an early stage and thus identify high-risk patients for GvHD-associated mortality. In the course of preliminary work bacterial metabolites were able to be readily detected that correlate significantly with survival. It is now intended that their predictive value will be multicentrically validated, the underlying pathophysiology studied in greater detail, and potential new biomarkers identified in the blood.
Prof. Dr. Weber is senior physician in the Department for Internal Medicine III at University Hospital Regensburg with a focus on allogeneic stem cell transplantation. Her studies in medicine and training as a specialist in hematology and internal oncology were equally completed in Regensburg. Since 2012 she has been conducting research in the field of allogeneic stem cell transplantation and successfully concluded her postdoctoral teaching credentials in 2019. “The concept of reentry funding following parental leave poses a great opportunity to create the necessary temporal space for work on scientific projects alongside clinical and family commitments so that the balancing act between profession and family can be a success,” explains Prof. Dr. Weber, who has two children.
In 2024 EKFS will once again announce a call for applications for the Else Kröner Clinician Scientist Return-To-Work Grant.
Else Kröner-Fresenius-Stiftung (EKFS) – Advancing research. Helping people.
Else Kröner-Fresenius-Stiftung is a non-profit foundation dedicated to the funding and advancement of medical research and the support of humanitarian projects. To date the foundation has funded around 2,400 projects. With an annual funding volume currently amounting to over 60 million euros it is the largest foundation in Germany that actively funds and supports medicine. You can find more information at: www.ekfs.de
Press Contact
Else Kröner-Fresenius-Stiftung
Bianka Jerke
Presse- und Öffentlichkeitsarbeit
Tel.: + 49 6172 8975-24
eMail: b.jerke@ekfs.de